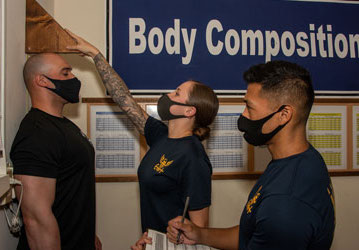
Your body composition is comprised of the different types of tissues and fluids—bone, muscle, fat, internal organs, skin, blood, and more—that make up your total body mass. To simplify this, body composition is broken into two components: lean, fat-free mass (muscle, bones, internal organs), and fat mass. Your body-fat percentage (BF%) is how much of your total body composition is fat mass. Fat mass is the easiest component to measure, and it has the most well-defined critical high and low percentages associated with adverse health effects.
Body fat is essential for normal body functions, especially for women who require more body fat than men to produce reproductive hormones. However, there is an upper limit to body fat where it becomes unhealthy. Higher levels of body fat are associated with long-term disease risk such as heart disease, various forms of cancer, and high blood pressure.
Obesity caused by excess body fat can lead to hormone dysfunctions. For example, leptin—the hormone that controls when you feel full when you eat—is produced in your body fat. But if you have too much body fat, your body becomes less sensitive to leptin. (This is similar to how your body is less sensitive to insulin if you have Type 2 diabetes.) This contributes to a vicious cycle of overeating because you don’t feel full. Then your body produces more fat from taking in too many calories, thus continuing leptin insensitivity.
For optimal military fitness, it is important to maintain a healthy level of body fat. Too much, or too little, body fat can have a negative effect on performance and can lead to long-term risk of chronic disease.
High levels of body fat can also hurt your quality of life, which can lead to conditions such as back and knee pain. This makes it difficult to perform everyday functions because you carry around extra weight that doesn’t improve your strength or mobility.
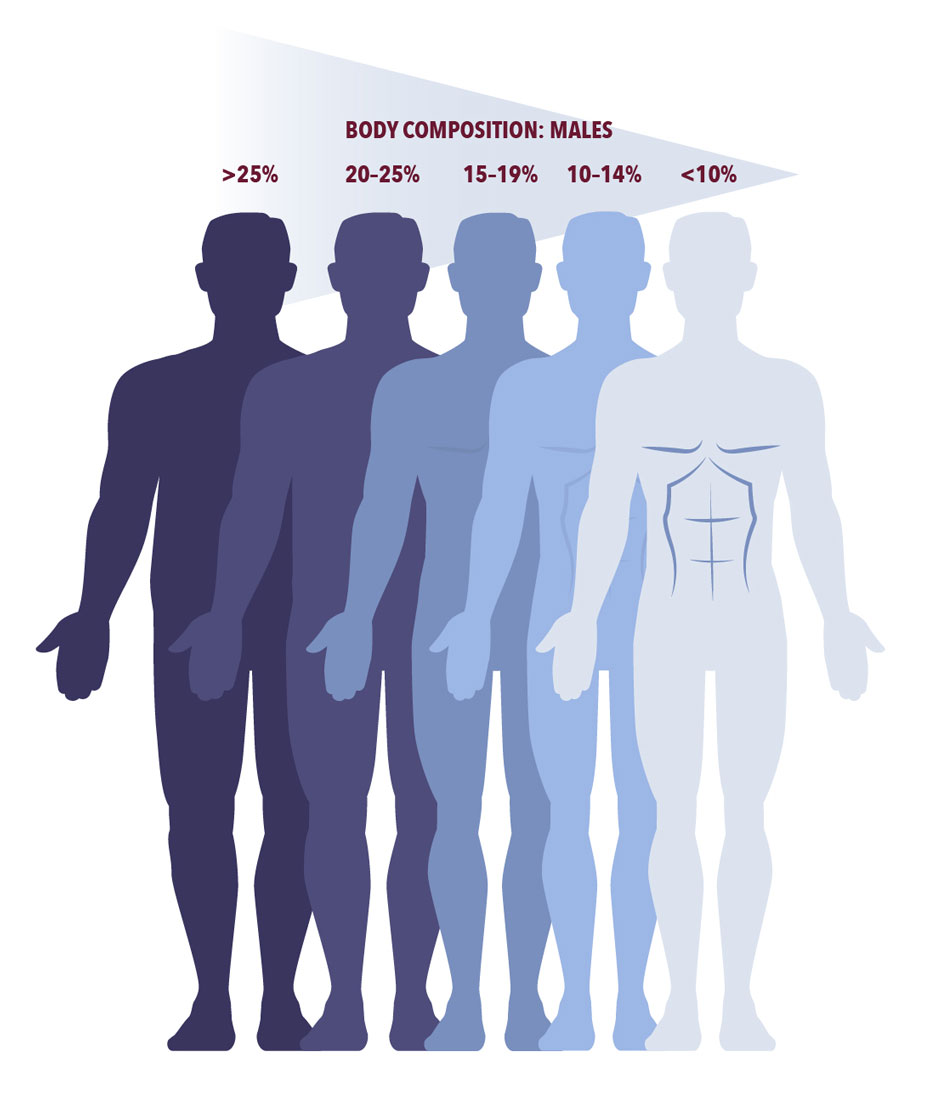
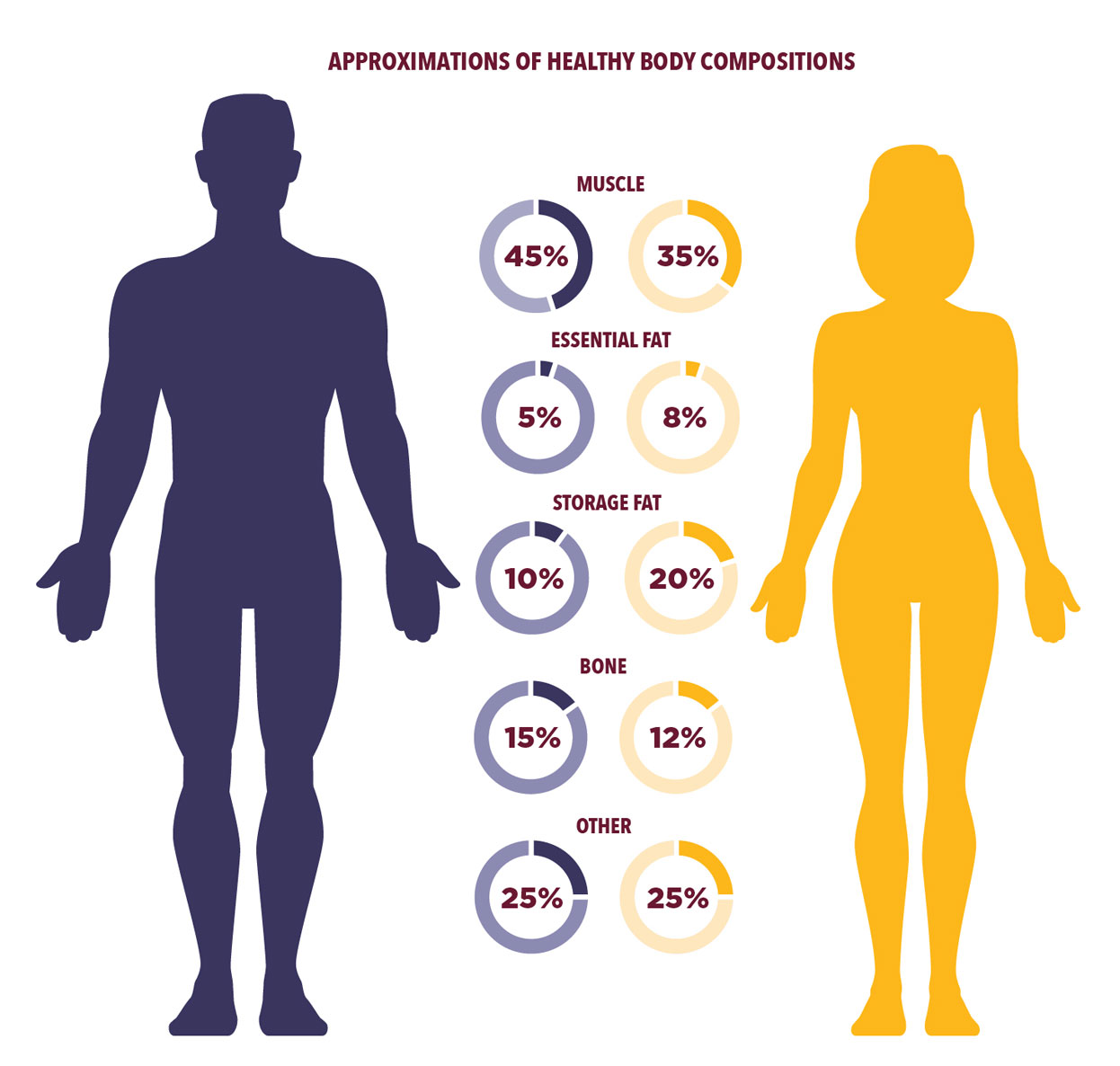 The “ideal” body fat percentage (BF%) is a wide range that changes based on your age and activity level. For young men, a healthy BF% is about 10–20%, and up to 25% for middle-aged men. The ranges are higher for women—15–30% for young women, and up to 38% for middle-aged women.
The “ideal” body fat percentage (BF%) is a wide range that changes based on your age and activity level. For young men, a healthy BF% is about 10–20%, and up to 25% for middle-aged men. The ranges are higher for women—15–30% for young women, and up to 38% for middle-aged women.
Some athletes are encouraged to be on the low end of their healthy ranges because it might benefit athletic performance. For example, endurance athletes usually have a very lean body composition because of their high level of energy expenditure and fat utilization during their long exercise sessions. A competitive male marathon runner will almost never have 20–25% body fat. Competitive bodybuilders—who display extreme levels of muscle size and definition—will cut their body fat below 10% (sometimes as low as 5%) for short periods of time around their competitions. It’s impossible to maintain this extreme body composition, and it provides little to no functional benefit.
Your body uses mostly fat for energy when you’re not exercising, so there is a minimum level of body fat you need even to sit at rest. Percentages below 5% for men and 8% for women are considered unhealthy—this is the minimum body fat required for basic life functions such as hormone production, fat-soluble vitamin absorption and storage (vitamins A, D, E, and K), and body-temperature regulation. For women, too little body fat leads to irregular menstrual cycles and difficulty getting pregnant. Experts say that about 17% body fat is the minimum level needed to menstruate, and 22% is the minimum for a regular cycle. Estrogens—the female sex hormones that regulate menstruation—are converted from androgens (male sex hormones) in fat tissue. This is why a minimum fat level is needed for normal menstrual function.
In addition to reproduction, the sex hormones (androgens, estrogens, and progestogens) are responsible for body functions such as bone and muscle growth. Men and women with too little body fat can experience abnormal sex-hormone production. Poor bone health and other negative effects related to relative energy deficiency in sport (RED-S) are tied to sex-hormone function, especially in physically active people.
Body-fat percentage for abs
If your goal is 6-pack abs, you need low levels of body fat to see them—less than 15% for men and less than 20% for women. A strict eating and exercise plan is needed to maintain these low levels of body fat, which can be difficult to sustain in the long term. While some might find visible abs physically attractive, it has little functional benefit. The purpose of the rectus abdominus muscle—the “6-pack abs”—is primarily to forward-flex the spine and limit backward hyperextension, while rotating your pelvis backwards. Secondarily, the rectus abdominus assists with breathing, which helps you forcefully exhale. Seeing the muscle has little bearing on its ability to function.

Ideal body-fat percentage
How do you determine your “ideal” body composition? The best place to start is to be in the healthy range. For most people, exact body-fat percentage doesn’t matter, as long as it’s not excessively high or low. Some health conditions create a need for more specificity with your body composition. For example, most women need at least 22% body fat to menstruate regularly. Through discussions with your doctor, you might find that being closer to 25% body fat leads to the best cycle regularity. Unless your doctor diagnoses you with a special health condition, your ideal body composition is whatever allows you to feel and perform your best without resorting to drastic measures such as abnormal eating patterns, calorie restriction, or excessive exercise habits. Since everybody is different, there is no single ideal body-fat percentage to recommend within the healthy range. Some people might be comfortable and perform well near the low end of healthy, others in the middle or even the high end.
DoD Instruction (DoDI) 1308.3 sets the basic rules for how strict military body fat standards can be. The maximum BF% set by the Services must be within 18–26% for men and 26–36% for women. However, specific body-fat standards vary by branch. For information on how BF% is measured, read HPRC’s article on measuring body composition.