- Adler, A. B., Britt, T. W., Castro, C. A., McGurk, D., & Bliese, P. D. (2011). Effect of transition home from combat on risk-taking and health-related behaviors. Journal of Traumatic Stress, 24(4), 381–389. doi:10.1002/jts.20665
- American Academy of Sleep Medicine, & Sleep Research Society. (2015). Recommended amount of sleep for a healthy adult: A joint consensus statement of the American Academy of Sleep Medicine and Sleep Research Society. Journal of Clinical Sleep Medicine, 11(6), 591–592. doi:10.5664/jcsm.4758
- Caldwell, J. L. (2002). Efficacy of napping strategies to counter effects of sleep deprivation, in Sleep/Wakefulness Management in Continuous/Sustained Operations (pp. 4.1–4.11). Neuilly-sur-Seine Cedex, France: North Atlantic Treaty Organisation, Research and Technology Organisation.
- Loprinzi, P. D., & Cardinal, B. J. (2011). Association between objectively-measured physical activity and sleep, NHANES 2005–2006. Mental Health and Physical Activity, 4(2), 65–69. doi:10.1016/j.mhpa.2011.08.001
- Toblin, R. L., Clarke-Walper, K., Kok, B. C., & Thomas, J. L. (2012). Energy drink consumption and its association with sleep problems among U.S. service members on a combat deployment—Afghanistan, 2010. Morbidity and Mortality Weekly Report, 61(44), 895–898.
- Roehrs, T., & Roth, T. (2001). Sleep, sleepiness, sleep disorders and alcohol use and abuse. Sleep Medicine Reviews, 5(4), 287–297. doi:10.1053/smrv.2001.0162
- United States Department of Agriculture Agricultural Research Service. (2016). USDA Food Composition Databases. Retrieved 10 March 2022 from National Agricultural Library
- National Institute on Alcohol Abuse and Alcoholism. Alcohol’s effects on the body. Retrieved 26 April 2017 from https://www.niaaa.nih.gov/alcohols-effects-health/alcohols-effects-body
- Barlas, F. M., Higgins, W. B., Pflieger, J. C., & Diecker, K. (2013). 2011 Department of Defense health related behaviors survey of active duty military personnel. TRICARE Manage Activity, United States Coast Guard, Fairfax, Virginia. Retrieved from: https://www.documentcloud.org/documents/694942-2011-final-department-of-defense-survey-of.html
- Boyko, E. J., Seelig, A. D., Jacobson, I. G., Hooper, T. I., Besa Smith, Smith, T. C., & Crum-Cianflone, N. F. (2013). Sleep characteristics, mental health, and diabetes risk: A prospective study of U.S. military service members in the Millennium Cohort Study. Diabetes Care, 36(10), 3154–3161. doi:10.2337/DC13-0042
- Jacka, F.N., Maes, M., Pasco, J.A., Williams, L.J., & Berk, M. (2012). Nutrient intakes and the common mental disorders in women. Journal of Affective Disorders, 141(1), 79–85. doi:10.1016/j.jad.2012.02.018
- Kennedy, D.O., Veasey, R., Watson, A., Dodd, F., Jones, E., Maggini, S., & Haskell, C.F. (2010). Effects of high-dose B vitamin complex with vitamin C and minerals on subjective mood and performance in healthy males. Psychopharmacology, 211(1), 55–68. doi:10.1007/s00213-010-1870-3
- Howatson, G., Bell, P.G., Tallent, J., Middleton, B., McHugh, M.P., & Ellis, J. (2012). Effect of tart cherry juice (Prunus cerasus) on melatonin levels and enhanced sleep quality. European Journal of Nutrition, 51(8), 909–916. doi:10.1007/s00394-011-0263-7
Key Points
- Emphasize rest and rejuvenation upon return from deployment to re-optimize your mental and physical performance.
- Consistently getting quality sleep is essential to recover from deployments.
- Good nutrition and regular exercise are excellent antidotes to stress.
- Avoid binge eating and drinking upon returning from deployments. Excess food and alcohol intake can lead to unwanted weight gain and is detrimental to your overall health.
Warfighters who have been away from home for extended periods of time for deployments and training missions probably need to recalibrate basic health behaviors when they return home. During those times away, food and beverage options might not always be optimal. You might experience weight loss or weight gain during deployment depending on access to nutritious food, opportunities to exercise, and your body’s response to stressful situations. Upon returning home, many Warfighters overindulge in food and alcohol, which can impact the ability to perform well. This chapter explores the web of connections between stress, sleep, exercise, and nutrition and how this can impact your health during reintegration.
The return home
While on deployment, Warfighters have to adjust their sleep and nutrition habits to meet mission constraints and limitations that come with being downrange. But habits that were helpful in theater might be harmful in a garrison environment.1 Many military personnel have concerns about their eating and drinking behaviors upon returning home after a deployment. Stress from deployment can sometimes lead to unhealthy nutrition decisions that add greater stress to an already hectic transition. For some Warfighters, weeks or months away from home also can result in feelings of having been deprived of comforts, which might promote binge eating and drinking. Significant problems—such as weight loss and/or gain, alcohol dependency, domestic problems, and even work-related conflicts—might occur that can affect overall military performance and general health and well-being.
Reintegration and stress
Reintegration back home can feel hectic, and dealing with your own stress as well as the stress of your family can create even more stress. You might struggle to adapt to routines that developed in your absence, cope with the loss or injury of a teammate, or return to your role as a parent. Loved ones at home might feel stressed asking about your experiences or just bringing you back into the fold on the home front. Each of you perceives your own particular stressors as very important, and it can be difficult f to understand one another.
Upon returning from combat, Warfighters often use alcohol and drugs to reduce stress, but these solutions provide only short-term relief from stress and actually contribute to stress over time. Stress also can make you more likely to smoke, have poor dietary habits, and be physically inactive. Extreme untreated stress lingering from combat can lead to violent, abusive, or threatening behaviors. And chronic stress can disrupt the body’s normal patterns, putting you at greater risk for illness, injury, and mental health issues.
Conversations with healthcare professionals and fellow Warfighters about deployment experiences are healthy and can be cathartic. Military commands have embedded operational, combat-focused psychologists who are familiar with unit missions, demands, and lifestyles and are available to speak with you at any time. In addition, Family Services are available on Navy, Marine Corps, Army, and Air Force bases. These services provide resources to help manage stress, relationships, money, and family and other personal issues.
It’s important to remember that not all stress is bad. Change and stress are inevitable, but they often provide opportunities for growth and development. Paying attention to sleep, physical activity, and nutrition provide a foundation for effective stress management and maximize your opportunities for post-deployment growth.
Sleep and rejuvenation
Most operations away from home prevent optimal sleep, so getting high-quality, restorative sleep should be high on a Warfighter’s priority list upon returning home. In fact, rest is one of the most important aspects of recovery, especially during times of change and transition. The mental and physical stressors of deployment might make it necessary to reset your stress-response system upon returning home. Lack of sleep, stress, and inadequate nutrition disrupt your body’s finely regulated internal systems. You need time off when you return from deployment to reconnect with family and friends, normalize routines within the household, and recover both mentally and physically. But many Warfighters returning home from deployments experience a variety of behavioral and emotional responses—including sleep problems—related to their war experience and combat occupational stress.
Insomnia, nightmares, and sleep disturbances are common, as the often-unpredictable environment and thoughts of the war zone can disturb sleep cycles, sleep quality, and sleep quantity. Sleep disturbances also are core features of the most common post-deployment mental health diagnoses, including post-traumatic stress disorder (PTSD), depression, and traumatic brain injury (TBI). Sleep is vital to re-establish the normal daily patterns needed for optimal mental and physical performance, immune function, and growth. Sleep loss also can be a risk factor for the development of a number of mental-health issues, including panic disorders, PTSD, depression, and suicide.
While the amount of sleep needed varies among individuals, most adults should regularly sleep 7 or more hours per night for optimal health.2 The time of day you sleep depends on circadian rhythms regulated by your brain. Circadian rhythm is linked to core body temperature, so the best time to sleep is at night, including the hours between 0300 and 0500 when core body temperature is lowest.3
Whether deployed or in garrison, Warfighters often don’t have control over how much and when they sleep. To perform optimally under such conditions, you need to be aware how your sleep habits impact your ability to be mission-ready. Once you’re aware and mindful of what can disrupt your sleep, you can take an active role in cultivating healthy sleep habits to take advantage of the time you do have to recover.
Sleep disruptors
Many factors, including some within your control, can prevent a good night’s sleep:
- Caffeine blocks the receptors that trigger sleep, so limit your intake and avoid it at least 4-6 hours before bedtime.
- Nicotine acts as a stimulant and decreases your ability to fall asleep. In addition, nicotine withdrawal might cause early awakening.
- Alcohol is a sedative that prevents deep, restful sleep.
- Pain and pain relievers. Some pain relievers contain caffeine, but if your pain is severe enough to interfere with your sleep, then it might be worthwhile to take one. Work with your healthcare provider to find what works best for you.
- Exercise, done regularly (at least 150 minutes each week), can improve sleep quality.4 For some people, exercising too close to bedtime might interfere with sleep, but you can experiment to find what schedule works best for you and your body.
- Medications such as decongestants, steroids, and beta-blockers can reduce restorative sleep.
- Late-night eating might throw off your body’s internal clock and keep you awake.
- Electronic devices such as smartphones, tablets, and computers give off “blue light,” which can disrupt sleep. Avoid them within 2 hours of bedtime if possible.
Mission priorities often give Warfighters little choice but to exercise close to bedtime, eat late at night, and engage in other kinds of behaviors that disturb sleep while deployed. Among Warfighters, common sleep disruptors such as caffeine and nicotine are widespread downrange and often help Warfighters perform optimally. However, habitual use of caffeine (such as from energy drinks) and tobacco is difficult to change and can contribute to sustained sleep problems upon returning home.5
Healthy sleep habits
A very important habit you can develop, especially when you’re back home, is to prepare your body, mind, and space for good sleep. Consider these preparations:
- Take a warm bath or shower before bed.
- Find a therapeutic pillow that cradles your neck and allows you to sleep on your side.
- Make your bedroom a place to sleep, so your body knows it’s a place for rest.
- Making certain your bedroom has adequate airflow and isn’t too hot or too cold.
- Use a fan to block out potentially disturbing noises.
- Dim the lights; darkness tells your body it’s time to sleep.
- Turn off all electronic devices at least 2 hours before bed.
- Follow the same relaxing sleep ritual every night.
You can use questionnaires such as the Epworth Sleepiness Scale to assess the overall quality of your sleep and your risk of experiencing daytime sleepiness due to poor sleep. Tracking your sleep also can help you be more aware of patterns that help or hurt your sleep habits. Try a sleep log such as HPRC’s two-week sleep diary or a sleep-tracking function on a mobile or wearable device to shed light on your existing sleep routines and factors that might impact your quality of sleep. To learn more about how sleep impacts Warfighter performance and how to combat sleep debt, visit HPRC’s sleep infographic.
Physical activity
Physical activity can effectively relieve stress. The act of physical exertion causes your body to release chemical substances (endorphins) similar in nature to opiates (sleep-inducing chemicals). Endorphins make you feel good and have no adverse effects, unlike many drugs. Regular exercise should be a scheduled part of any returning-home plan. It even can be in the form of enjoyable recreational activities such as camping, hiking, basketball, cycling, running, or weight lifting. You can share exercise activities with family members and friends too, helping your reintegration process. Or you can use exercise to create “alone time” if you need it. Making room for exercise will help keep life issues under control and promote relaxation.
Learn more about exercise to improve your endurance, strength, and flexibility.
Alcohol
Post-deployment, Warfighters often turn to alcohol to cope with stress and insomnia.6 In fact, returning home from deployment is a common time for alcohol abuse to surface. However, alcohol provides no nutritional value, and it’s high in calories (see Table 15-1), even more so when mixed with sugar-sweetened beverages such as soda or juice.
Table 15–1. Caloric content of alcoholic beverages7*
| Alcoholic Beverages | Serving Size (ounces) | Total Calories |
|---|---|---|
| Beer | 12 | 153 |
| Light beer | 12 | 103 |
| Red wine | 5 | 125 |
| White wine | 5 | 121 |
| Dessert wines | 3.5 | 157–165 |
| Distilled spirits (gin, rum, vodka, whisky; 90 proof) | 1.5 | 110 |
| Mixed drinks | 8 | ** |
*Content can vary with brand or variety.
**Mixed drinks can contain even more calories due to the addition of soda, juice, and/or syrups.
Furthermore, alcohol affects mental health and performance, making it more difficult for a Warfighter to readjust to home life. Heavy alcohol consumption can have other negative effects on the body:
- Liver. Your liver processes alcohol, which is why so many alcoholics and heavy drinkers experience liver damage that might not be reversible.
- Pancreas. Alcohol also can damage your pancreas, which is involved in digestion. Pancreas damage can affect what you’re able to eat and drink.
- Heart. Alcohol increases blood pressure and puts you at risk for stroke and cardiovascular disease.
- Immune system. Excessive drinking puts your immune system at risk, so you’re more susceptible to infections and diseases such as cancer.
How much alcohol is acceptable?
Drinking 1–2 servings of alcohol per day is considered moderate. See Table 15–1 for typical single-serving sizes. For many people, red wine in moderation (2 drinks a day for men and one drink a day for women) can increase good cholesterol (HDL) and protect from heart disease. However, beyond these amounts, alcohol has many harmful effects.8
Binge drinking
Approximately one-third of active-duty Military Service Members report binge drinking.9 Binge drinking is defined as a pattern of drinking that leads to a blood alcohol concentration of 0.08 g/dL or more.8 In practical terms, this means 5 or more drinks for men and 4 or more drinks for women in a period of about 2 hours. Repeated intoxication prevents full participation in normal activities and fulfillment of other obligations and significantly increases the risk for alcohol-related hospitalizations. Binge drinking is a sign of being overstressed.
To learn more about the dangers of binge drinking and how to get help, visit Military OneSource.
Putting it all together with Total Force Fitness
Health behaviors are all interconnected. Total Force Fitness (TFF) is the concept that optimal performance requires a connection between mind, body, spirit, and family and social relationships. Eight domains make up TFF: physical, nutritional, medical and dental, environmental, behavioral, psychological, spiritual, and social. HPRC provides in-depth information and resources for most of these.
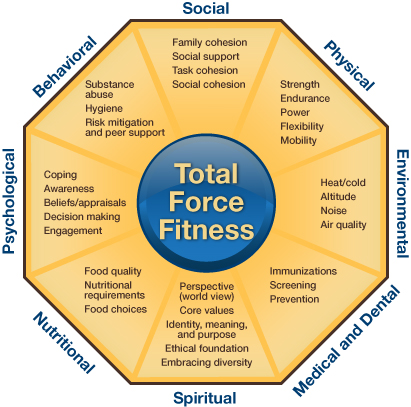
When your health in one domain takes a downturn, another domain likely will be affected, causing you to get stuck in a vicious cycle. Stress and insufficient sleep often go hand-in-hand because stress keeps you awake, and in turn, your inability to sleep might increase your feelings of stress. During sleep your body releases important hormones. If you don’t get enough sleep, the altered levels of these hormones can have serious repercussions for your health and well-being, including increased risk of obesity, diabetes, cardiovascular disease, and mood disturbances. Lack of sleep also affects your ability to make sound moral judgments and other decisions and regulate your emotions. It also increases cognitive impairments. Sleep loss even can affect your family and social relationships by lowering your ability to interact, communicate, and interpret the emotions of others.
Sleep impacts your eating habits too. Sleep deprivation can cause you to make poor food choices, which can increase your risk of diabetes.10 Shorter sleep times also are associated with higher Body Mass Index (BMI) and imbalances in the hormones that regulate hunger and appetite. Weight gain can give rise to sleep apnea and other issues that further negatively impact sleep, creating a vicious cycle.
Using nutrition to break the cycle
When you return home from deployment, you might go for “comfort” (high-fat and high-sugar) foods. Research continues to show strong relationships between nutrition and stress and between exercise and stress. A high-fat, high-sugar diet combined with chronic stress is a major factor in developing obesity. In contrast, meals rich in vegetables, fruits, whole grains, and lean protein provide essential nutrients that promote mental health and contribute to a healthy weight.11 The minerals zinc and magnesium and vitamins C, B complex, and E are important to combat stress.12 B vitamins and magnesium also are involved in producing serotonin, a hormone that helps regulate mood and relieve stress. Making wise food and exercise choices will promote faster readjustment when returning home from deployment.
Substances likely to aggravate stress include:
- Caffeine
- Alcohol
- Tobacco
- Fried and highly-processed foods
Around the world, traditional foods are served to promote healthy sleep. In many Western countries, a glass of warm milk or a cup of chamomile tea before bed is considered a tranquilizing beverage with sleep-inducing capability. Cherries are a natural source of the sleep hormone melatonin, and tart cherry juice has been found beneficial to improve sleep duration and quality.13 Tryptophan, found in foods such as turkey and pumpkin seeds, might affect sleep, but it depends on what else you eat at the same time. In general, it requires large amounts of tryptophan-containing foods to affect your sleep. Finally, almonds and spinach are rich in magnesium, which is known to promote sleep and relax muscles.
Taking care of yourself in all the domains of TFF is essential for optimal health, wellness, and resilience, especially if you’re a Warfighter returning home. Nutrition plays an integral part in recovery after deployment. Positive nutrition habits can promote positive changes in the other domains, leading to a successful return to home base.

